
Diagnostic Radiology Residency
The UW Diagnostic Radiology program accepts 11 residents per year for a total of 44 residents. There is also the opportunity to apply for two integrated Interventional Radiology residency positions.
Residents rotate in 4-week blocks through various Radiology subspecialties over the four years in a variety of clinical settings including the University of Wisconsin Hospital, American Family Children’s Hospital, and the Veterans Administration. Structured experiences with progressive independence allow growth and capability for independent functioning at the conclusion of the program.
Thank you for your interest in the radiology residency program at the University of Wisconsin School of Medicine and Public Health. We have a vibrant program driven by renowned faculty and talented residents. Our department is committed to the academic, professional and personal development of our trainees. We recognize that our most important asset is our community and its members – including attendings, trainees and our support staff of technologists, nurses and administrative assistants.
We continue to iterate our approach to clinical care and education, maintaining a robust experience in both common pathologies and imaging techniques, as well as exposure to next level research and cutting-edge technologies. Our residents graduate from this program well-equipped for a successful career, no matter their future path, and with many wonderful lifelong friends and colleagues.
Sincerely,
Allison Grayev, MD (Program Director)
Mitchell Daun, MD; David Kim, MD, FACR, FSAR and Timothy Ziemlewicz, MD (Associate Program Directors)
Admissions/Application Criteria and Interview Information
University of Wisconsin Department of Radiology accepts individuals from LCME accredited medical schools who have demonstrated that they have achieved the criteria listed below. Individuals are selected based on merit and there is no discrimination based on gender, ethnicity, race, cultural background, or disability.
- The individual has achieved at least average evaluations in all clinical rotations and in key pre-clinical courses.
- The individual has shown sufficient knowledge based on clinical grades and USMLE/COMLEX pass rates to be able to function at the level of a PG2 in this program.
- The individual has consistently had positive comments and no serious negative comments regarding their professional, ethic, and work habit skills.
- The individual has had training in an institution where the individual has developed sufficient knowledge of language and interpersonal skills as well as cognitive, technical, attitudinal, and professional skills to be able to learn radiologic interpretation and perform image-guided intervention.
- The individual has not had evidence of academic difficulty or a hiatus that has been too long to allow them to function in a clinical arena without demonstration of subsequent competent performance in a relevant clinical environment.
- Meets all hospital admission policy standards.
- Application materials should be submitted through ERAS at http://www.aamc.org/eras by the date before ERAS opens for programs, so the 4th Tuesday of September. Applications will be considered complete when we have electronically received the following items:
- completed ERAS application, including a brief (one page or less) personal statement indicating your goals and reasons for selecting a radiology residency (please indicate your level of interest in our program)
- three (3) letters of recommendation
- medical school transcripts
- USMLE Step 1 or COMLEX-USA Level 1 pass rate
- Medical School Performance Evaluation (MSPE – Dean’s letter)
- Program Signals: We are accepting program signals. We encourage students interested in one of our programs to signal as signaling is a factor we consider when extending interview offers. For the applicants who are applying to both the DR program and the IR-Integrated program, we consider a signal to either program to be a signal of interest in our institution and UW Radiology in general. Thus, we recommend signaling either the DR or the IR-Integrated program depending on which you consider to be your primary interest. Due to the configuration of our selection committee and combined interview process, both programs will know if you signaled the other. For instance, if you signal IR-Integrated and applied to both the IR and DR programs, the DR program will be aware of your signal to IR and hence your interest in BOTH programs with a preference for IR. The converse is also true if you signal DR.
The Department of Radiology adheres to the UW Health Graduate Medical Education eligibility criteria for foreign medical graduates. Applicants who are not US citizens must acquire or currently hold one of the following to begin training at UW Health in an ACGME accredited residency or fellowship program.
- Lawful Permanent Resident (“Green Card”)
- Initial or continuation of a J-1 visa which is sponsored by the Educational Commission for Foreign Medical Graduates (ECFMG) for the sole purpose of Graduate Medical Education training (you do not need to be fully ECFMG certified by application submission)
- Employment Authorization Document (EAD)
For additional information, please review the GME eligibility for non-US citizens document and visit the GME credentialing and conditions of employment page.
- Recommendation from Program Director with a performance summary
- Summary of actual evaluations in prior GME program and list of completed rotations
- Full PG1 Application
- Explanation of reason for transfer
- Updated Curriculum Vitae
- Letter from two GME supervising attendings
- Milestones Achievement Summary
Interviews
Invitations to interview will be sent out no later than mid-October. Interviews are conducted November-January.
We interview for 13 radiology residency positions (11 Diagnostic Radiology positions and two IR-integrated positions). All 13 of the radiology positions are advanced track positions, which begin at the PGY2 level following the completion of an internship year. Diagnostic Radiology offers four preliminary positions (PGY1), two with Internal Medicine and two with General Surgery, all at UW Health. IR-Integrated also offers one General Surgery preliminary position at UW Health. The preliminary years include 2 months spent with the UW Department of Radiology. You do not need to apply separately to the preliminary programs, and there is not a separate interview for the preliminary positions. You will need to rank the UW preliminary program at the time of your list submission on your supplemental rank order list if you are interested in attending your preliminary year at UW. When it comes time to create your rank order list, you can rank all, some, or none of our positions below as you see fit:
- Diagnostic Radiology Advanced Track NRMP Program Code: 1779420A0
- Diagnostic Radiology Internal Medicine Prelim year NMRP Program Code: 1779140P2
- Diagnostic Radiology General Surgery Prelim year NMRP Program Code: 1779440P4
- IR-Integrated Advanced Track NMRP Program Code: 1779416A0
- IR-Integrated General Surgery Prelim year NRMP Program Code: 1779440P5
Program Highlights
Resident Tracks
Early Specialization in Interventional Radiology (ESIR) Pathway this residency pathway allows a DR resident to specialize in interventional radiology during their diagnostic residency training program. The ESIR pathway will consist of a full year of interventional radiology specific training in their fourth year of residency. Residents who complete the ESIR rotations and the required 500 patient procedural encounters will be eligible to start in an advanced position in an independent program to which they match for their fifth year of training. This training will allow the resident to sit for the dual interventional and diagnostic radiology boards. Applications will be submitted and reviewed in the second year of diagnostic residency training.
Nuclear Medicine 16-Month Pathway this residency pathway allows a DR resident to complete 16 months total of nuclear medicine or related rotations during their DR training. This will enable the DR resident to sit for dual subspecialty certification in nuclear medicine (ABR Nuclear Radiology) and diagnostic radiology. Four months of nuclear medicine rotations are already required as part of the DR rotation curriculum and will count towards the 16 months of experience. Eight additional months of dedicated nuclear medicine comprise 12 months, where up to four of the remaining months of training may be in a field related to nuclear medicine. Examples of related fields include: abdominal/cardiovascular, musculoskeletal, thoracic radiology, head and neck, neuroradiology, interventional radiology, non isotopic molecular imaging and oncologic imaging. Applications will be submitted and reviewed in the second year of diagnostic residency training.
Pediatric Radiology 15-Month Pathway this residency pathway allows a DR resident to complete 15 months total of pediatric radiology or related rotations during their DR training. This will enable the DR resident to sit for dual subspecialty certification in pediatric radiology (ABR Pediatric Radiology) and diagnostic radiology. Three months of pediatrics rotations are already required as part of the DR rotation curriculum and will count towards the 15 months of experience. Eight additional months of dedicated pediatric radiology comprise 12 months, where up to three months may be focused on either additional subspecialty training within pediatric radiology or in areas outside of pediatric radiology to gain technical expertise applicable towards pediatric patients. For example, gaining expertise in adult-oriented cardiac imaging that includes patients with treated congenital heart disease. Applications will be submitted and reviewed in the second year of diagnostic residency training.
Research Track Resident this track is intended to facilitate the career of a resident planning on an academic career. Applications are due January of R1 year. The selected resident will choose a research mentor. A mentoring committee, including the resident identified research mentor will provide oversight (annual meetings to develop goals as well as review the past year) and help facilitate relationships with the larger research community outside of UW. The research residents will have regular academic days (2 per month) during the R2-3 years and research month electives in the R4 year. The expectation includes regular presentations at national and subspecialty meetings and publications by the resident.
Clinical Experience
The clinical experience sets a solid foundation for the resident.
A variety of clinical settings, from the University Hospital and specialty clinics such as the Digestive Health Center to the Children’s hospital and the VA, lead to a wide-ranging, comprehensive experience for the resident.
As residents advance in the program, they assume progressive responsibility in the imaging care of the patient. Teamwork, communication, and collegiality are core tenets in the workplace.
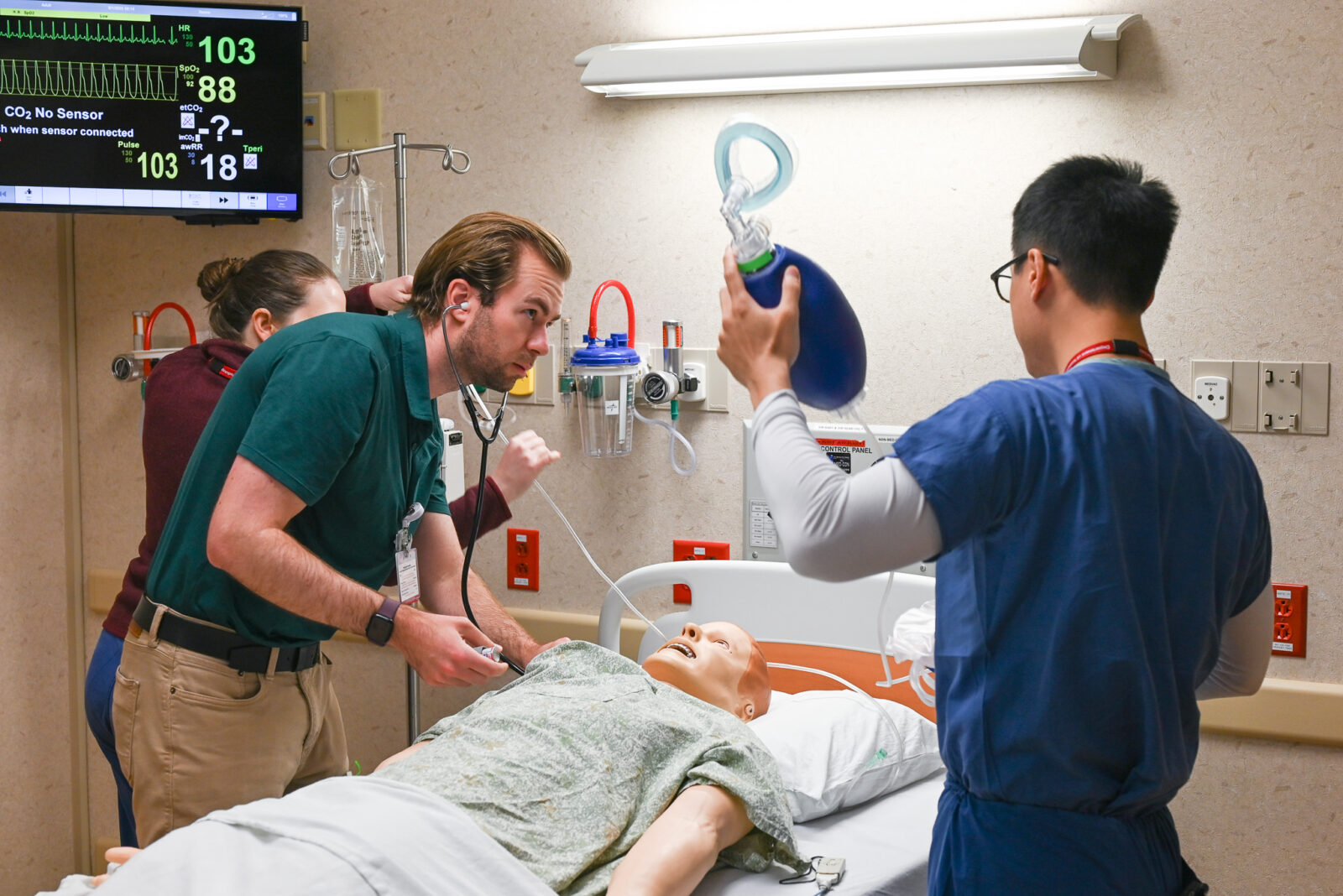
Rotations

The residents rotate through the various subspecialties of Radiology in four week blocks.
Residents assume progressive responsibility where they are expected to “run” the service in their more senior years from protocoling and managing service workflow and patient issues to answering questions “imaging consults” for referring providers. Extensive daily in-person feedback and in-house developed evaluation tools help a resident to gauge their growth.
Highlights:
Emphasis on ultrasound scanning skills. Multiple scanning opportunities in several rotations as well as an ultrasound scan lab. (See more information under the Procedures tab.)
Excellent clinical programs drive a robust imaging experience in all areas of Radiology for residents. Internationally recognized expertise at UW leads to specific experiences difficult to get at all programs. For example, the CT colonography screening program allows residents to set a solid foundation in CTC interpretation.
Strong emphasis on procedures. Image-guided procedures are incorporated in each subspecialty, allowing for procedural experience throughout the year in addition to formal interventional rotations.
Procedures
Residents undertake procedures as a component of many rotations outside of their dedicated interventional rotations. Each subspecialty performs procedures as part of their clinical service.
For example, the MSK section undertakes joint aspirations and injections as well as bone biopsies whereas the abdominal section performs image-guided biopsies of masses in the chest and abdomen, paracenteses, and thoracenteses. Neuroradiology undertakes fluoroscopic-guided lumbar punctures.
These experiences allow for a strong foundation in procedural technical skills over the course of the residency. Besides procedures, ultrasound scanning is emphasized with dedicated labs and clinical experiences to allow a resident to become proficient in scanning.

Ultrasound Scan Lab
The Ultrasound Scan Lab is a unique opportunity for our residents to practice ultrasound-scanning skills in a low stakes environment on volunteers and phantoms.
This course runs over eight-month period. Scanning sessions provide the residents with hands-on ultrasound skills and are facilitated by trained sonographers and subspecialty faculty.
Topics include:
- Knobology
- Abdominal ultrasound scanning techniques
- Vascular ultrasound
- Ultrasound-guided procedures
- Breast Ultrasound and Ultrasound-guided interventions
- Pediatrics Ultrasound exams
Call
Independent call is a key formative experience in a resident development as a Radiologist.
Unfortunately, a national trend has been towards 24/7 faculty coverage and loss of this educational opportunity. UW has worked hard to maintain this resident experience, working with ED, trauma surgeons, and hospital administration to convey the importance of this experience. We ensure that resident is able to handle this responsibility and provide appropriate oversight and support. We employ a team approach, particularly during the busy hours, allowing for several residents to work together.
Residents undergo rigorous preparation to become eligible for call, including a dedicated curriculum of call-specific lectures and interactive cases (‘Boot camp lecture series’). Competency testing ensures that the residents are ready for this experience where the residents must pass this call simulation prior to becoming eligible for independent call. On call, residents are monitored with call discrepancy rates and turn around times. We strongly believe that call is a transformative experience that is necessary to become the best Radiologist possible.
- Call Experiences The core of the independent call experience is night float. Residents work from 9 p.m. to 7 a.m. A senior short call (4:30 p.m. – 1 a.m.) allows for overlap of the busy times in the ED in the late evening. Residents interpret ED and emergent inpatient studies and are formally over-read in the morning. A junior call person works into the early evening (4:30 p.m.-9:00 p.m.), handling plain films and fluoroscopy. There are several subspecialty faculty on call each night for any questions if needed.
- Boot-camp Lectures This preparatory lecture series is geared toward typical diagnoses and imaging issues related to call. A mix of didactic and interactive case seminars are given over a 9 week period culminating in a pre call competency test.
- Pre-call Competency Test This 5-hour test is held over a period of one week (one hour per day). Each section involved in call (abdominal, chest/cardiovascular, musculoskeletal, neuroradiology, and pediatric radiology) provide a set of cases, mirroring the typical cases encountered during call. Residents review the anonymized images on a PACS station and dictate preliminary reports. Residents must pass all sections of the call simulation in order to be eligible to take independent call. Those residents conditioning a section of the test work with faculty to correct any deficiencies and must pass a secondary test before beginning call.
- Call Monitoring Residents are monitored by turn around times and call discrepancy rates. In house electronic applications have been created that allow realtime dashboards. In addition, resident receive faculty evaluation of the night float rotation.
Curriculum

The UW Department of Radiology has a well-developed comprehensive curriculum consisting of:
- Innovative lectures that provide residents with the foundations of imaging sciences, physics, and non-imaging interpretive skills. Specific content series have been developed to enhance resident learning and experience.
- Interactive case conferences and seminars to improve case taking skills.
- Rotation specific multi-disciplinary conferences.
- Opportunities for residents to participate as teachers.
Daily lectures are scheduled at 7:30 a.m. and 12:00 p.m. and are available for offsite residents through webcasting. All lectures are recorded and available for nonsynchronous viewing by the resident. Active optimization and curation of lectures are undertaken on an ongoing basis by a curriculum oversight committee comprised of faculty and residents.
Lecture Content Series
- Core Teaching Conference Series Structured content is provided from a subspecialty perspective where each section determines the core didactic topics to be covered over a two-year cycle with oversight by the Curriculum committee. Conferences are a mix of traditional lecture format, innovative new delivery systems, and interactive case seminars. This curriculum is continuously being evaluated to incorporate resident feedback, update the lectures within the series as well as incorporate emerging imaging technologies.
- Introduction to Radiology Lecture Series The 4-week didactic lecture series is geared towards PGY2 (R1) residents and takes place at the beginning of the academic year. This series of lectures introduces incoming residents to principles of image interpretation within each subspecialty of radiology.
- Resident Led Call Prep Series R3 and R4 residents go through call cases with R2 residents over a 4-week period to help prepare them for independent call. This series introduces residents to a wide array of cases they could encounter during call. This series takes place before the formal Call Prep Conference Series while the R1 residents are in their introductory lecture series.
- Call Prep Conference Series This 10-week didactic lecture series prepares residents for independent call. Topics covered include a wide array of radiologic diagnoses encountered during call.
- Radiology-Pathology Correlation Series This is a resident-led conference that is co-presented with Department of Pathology residents. The aim of this conference is to discuss the imaging and pathologic findings of interesting diagnoses and discuss their clinical implications.
- Multidisciplinary Teaching Conferences These are subspecialty clinical weekly/bimonthly conferences that are led by radiology faculty, fellows and senior residents. All residents are encouraged to attend these conferences when they are rotating on their designated rotations.
- Radiology Resident Medical Physics Course A resident curriculum provided by faculty in the Department of Medical Physics during the Core Teaching Conference Series and covers the fundamentals of medical physics.
- Imaging Informatics Leadership Program The Imaging Informatics Leadership Program (IILP) is a lecture series focused on imaging and clinical informatics topics that are open to residents and faculty interested in learning more about informatics topics. For individuals interested in diving deeper, there are opportunities to participate in ongoing or new informatics departmental projects.
- Professional Development Lecture Series Lecture series for residents to prepare them for a successful career in radiology. Topics include but are not limited to applying for fellowships, interviewing skills, career paths, contract negotiations, financial planning, and social impact and belonging initiatives.
Resident Research

Numerous quality opportunities for residents exist to participate in research projects with nationally and internationally renowned faculty.
Although not formally required, the majority of residents engage in research during their residency. Resident alumni note that the knowledge and skills gained from these experiences have been useful after residency whether in academics or private practice.
Highlights
- Extensive guidance and mentoring by faculty. It is a wonderful way to build lasting relationships.
- Department R&D funding available for resident projects.
- Strong support with time and funding to present at national and subspecialty meetings.
- Excellent ancillary services including statistical support.
Mentorship

Mentorship and career guidance is one of the cornerstones of success for our residents at the University of Wisconsin.
Formal Mentorship
- Clinical Competency Subcommittee Each class of incoming radiology residents are assigned a formal mentorship committee in the form of a Clinical Competency Committee (CCC) subcommittee, consisting of an Associate Program Director (APD) as chair and other education faculty mentors. This committee follows each class throughout residency with regularly scheduled group and individual meetings to discuss resident progress, education plan, selection of electives, research guidance, fellowship decisions and career opportunities.
- One-on-One Faculty to Resident Mentorship Each class of incoming radiology residents are assigned a faculty mentor within the first month of residency. The faculty member and resident will meet throughout the resident’s first year to help them navigate the radiology residency program landscape, answer any of their questions, and help guide them towards their specific interests in radiology.
- Big Sib/Little Sib Resident Mentorship Each class of incoming radiology residents are assigned a second-year resident mentor within their first couple of weeks of residency. The residents will meet periodically throughout the year to give the first-year resident insight into how to navigate their residency, give rotation tips and tricks, and answer any questions they may have.
- Peer-to-Peer Resident Mentorship Residents are split up into vertical “houses” consisting of a mixture of residents at each level of training. These groups meet periodically throughout the year to ensure each resident is learning from and able to ask questions of all levels of residents during their residency training.
Informal Mentorship
Residents highly value the role of informal mentorship that develops organically between mentors and mentees with well-aligned career interests and personalities. The collegial and welcoming department culture at the University of Wisconsin has fostered many of these informal mentorships throughout the years that resulted in lifelong collaborations and friendships.
Mentorship opportunities for Women Professionals in Radiology have been one of the main goals of our Social Impact and Belonging leadership with allocated department resources and support that fosters resident success.
Life Outside of Work




Our residents take advantage of the multitude of experiences and opportunities that Madison has to offer.
Madison is frequently listed as one of most livable cities in the country and whether you are interested in outdoor activities, sporting events, concerts, or enjoy eating out – Madison has something for everyone. The resident community extends beyond the hospital and residents often get together for trivia nights, Badger games, intramural sports, and shared extracurricular interests.
Highlights
- Big city perks with smaller city feel/livability
- Easy access to the outdoors (four lakes, miles of bike paths/hiking trails, 270+ parks)
- Lively departmental community (involving residents/fellows and attending alike)
- Expansive cultural opportunities (museums/performing arts, sporting events, live music, food & drink possibilities.
