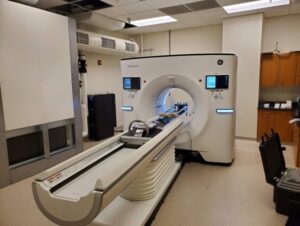
 The collaborative relationship between UW Radiology and GE Healthcare continues to spur on innovation in radiology. In the newest chapter of this partnership, beginning in November 2022, a prototype deep silicon photon-counting computed tomography (PCCT) scanner will be evaluated at the Wisconsin Institute for Medical Research (WIMR). This technology has the potential to improve both spatial and spectral resolution of CT imaging, a breakthrough that could increase imaging performance across care areas.
The collaborative relationship between UW Radiology and GE Healthcare continues to spur on innovation in radiology. In the newest chapter of this partnership, beginning in November 2022, a prototype deep silicon photon-counting computed tomography (PCCT) scanner will be evaluated at the Wisconsin Institute for Medical Research (WIMR). This technology has the potential to improve both spatial and spectral resolution of CT imaging, a breakthrough that could increase imaging performance across care areas.
The PCCT scanner is technology in development and represents ongoing research and development efforts. The scanner is not a product and may never become a product, and it is currently not for sale nor approved or cleared by the FDA or any other global regulator for commercial availability.
The project will be led by Timothy Szczykutowicz, PhD and Dr. Meghan Lubner, MD. Their study team – which includes Rachel Bladorn, Aria Salyapongse, Carrie Bartels, and Jan Yakey – has two main aims. First, they hope to provide feedback to GE engineers and scientists to guide future optimizations of the scanner to address clinical needs. To reflect this focus, the study team also includes radiologists from several subspecialities: Jeff Kanne, MD; Thomas Grist, MD; Prashant Nagpal, MD; David Bluemke, MD, PhD, MsB; Greg Avey, MD; Tabby Kennedy, MD; Brian Markhardt, MD; Nicholas Laucis, MD; Giuseppe Toia, MD; Perry Pickhardt, MD; and Myron Pozniak, MD.
Second, the study will assess the PCCT’s performance on the image quality issues that often affect conventional CT scanners. A normal CT scanner is based on energy-integrating CT (EICT) detection technology. Photon counting technology is entirely different, and has exciting possibilities for image quality and, therefore, diagnostic accuracy.
The study team will examine five specific aspects of the scanner’s performance.
1. Opportunistic screening describes how well the CT numbers of a subject can be determined as that subject’s size changes.
2. Noise streaking, the artifactual lines across a CT image due to low signal levels, may be reduced in the PCCT scanner, as compared to the conventional EICT scanner.
3. Calcium scoring measures the scanner’s ability to find and quantify the density and size of calcium in the body.
4. When metal is present in a CT scan, it causes large black and white bands on the image. Metal artifact reduction, or MAR, will measure the PCCT scanner’s imaging quality in the presence of metal.
5. The spatial resolution of the PCCT scanner will also be evaluated. Typically, the pixels in the middle of an image are sharp, with the image becoming less clear further away from the center.
Each of these features has a powerful effect on image quality, and therefore, diagnostic accuracy. To illustrate this relationship, consider the implications of improved calcium scoring, one of the five features above. Calcium is present in coronary arteries as plaques. A scanner with a greater ability to image calcium will more precisely locate these plaques. Consequently, a patient’s risk of coronary heart disease can be better classified.
The team at UW-Madison believe that this new method of scanning might be leveraged for better and more accurate diagnostics. Their study’s evaluation of the PCCT scanner is a crucial step towards improved imaging performance.
Listen to Dr. Szczykutowicz describe the work in this interview with Radiology Business.